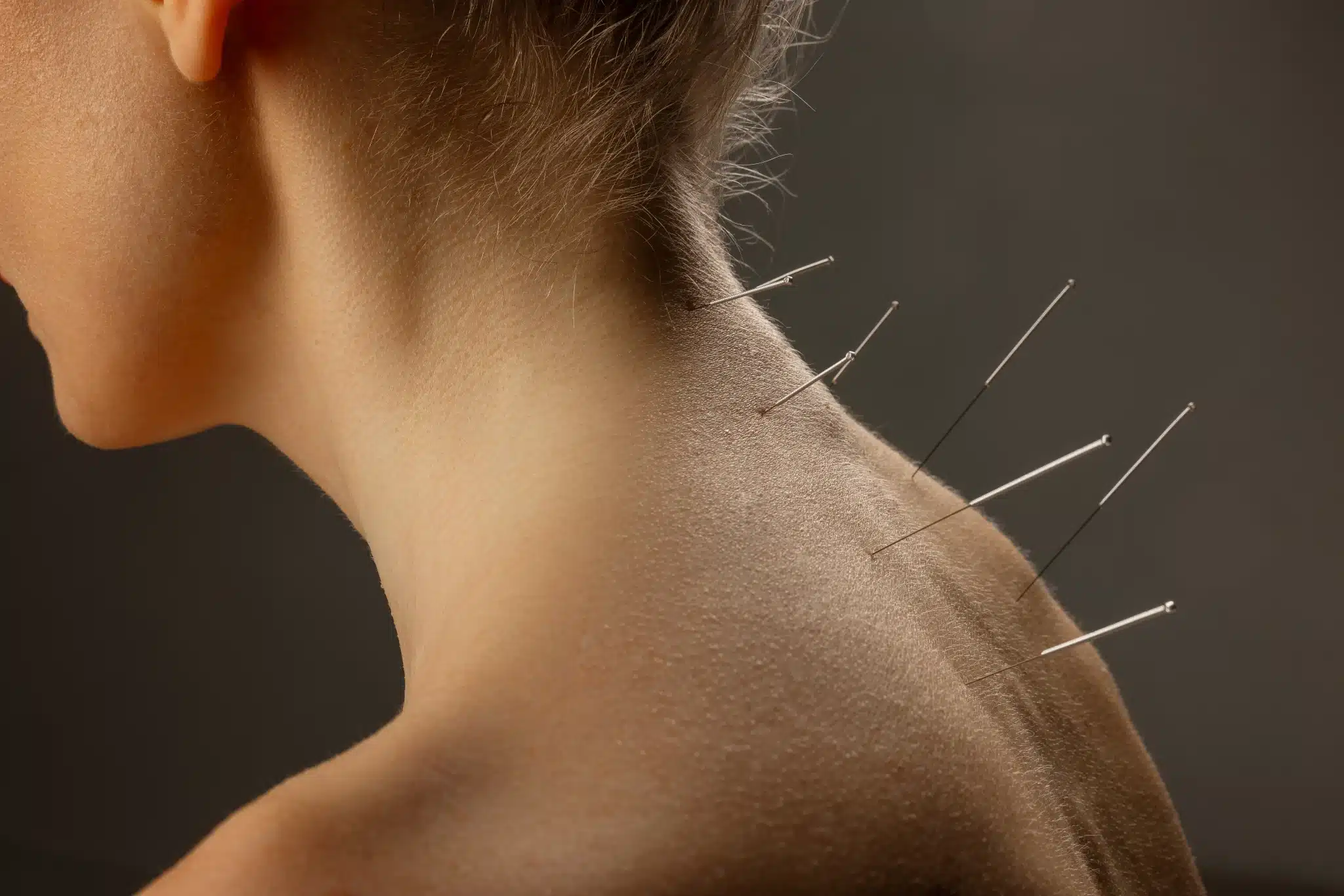
Medical billing and coding is a complicated, but necessary, process for both medical and holistic practices looking to be reimbursed for services. However, the world of medical billing processes can become rather complicated very quickly, with people throwing around a lot of technical terms that holistic practices may not be accustomed to hearing or dealing with. If your acupuncture practice plans on accepting insurance, you will need to become familiar with this terminology to maximize your insurance reimbursements and minimize denied claims.
You will frequently hear the following common acupuncture billing terms when dealing with insurance claims or working with an experienced acupuncture billing company like Holistic Billing Services. To ensure a streamlined acupuncture billing experience, keep this list handy in case you ever need to quickly reference unfamiliar acupuncture billing terms!
What is Acupuncture Billing?

Medical billing is the process of healthcare providers submitting claims with insurance companies in order to be reimbursed for their services. This can include anything from treatments, procedures, and testing. The medical billing process is essential for most practices to receive payments.
Acupuncture billing practices are not the same as traditional medical billing and have a different set of requirements. Before billing can be initiated, many holistic practices must first be credentialed with health insurance companies. On top of your holistic practice’s insurance enrollments, the right billing, coding, and SOAP documentation must be used.
Acupuncture billing uses its own unique set of codes. Since acupuncture services are always coded in 15-minute increments, you will use one code for the initial 15 minutes of service and then a separate code for additional units of time. Acupuncture CPT codes will only vary if you include electronic stimulation in your treatment.
Most Common Acupuncture Billing Codes
Many of the services your acupuncture practice will bill to insurance for treatments will fall under the following four codes:
Initial Acupuncture. Code: 97810. Initial 15-minute insertion of needles and personal one-on-one contact with the patient. (Tip: do not report this in conjunction with 97813; use one or the other).
Subsequent Unit of Acupuncture. Code 97811. Use one unit per each additional 15 minutes of personal one-on-one contact with the patient after the initial 15 minutes, with re-insertion of needles. (You may use it in conjunction with either 97810 or 97813).
Initial Acupuncture with Electrical Stimulation. Code 97813. Initial 15-minute insertion of needles, personal one-on-one contact with the patient. (Tip: do not report in conjunction with 97810; use one or the other).
Subsequent Unit of Acupuncture with Electrical Stimulation. Code 97814. Use one unit per each additional 15 minutes of personal one-on-one contact with the patient, with re-insertion of needles. (You may use it in conjunction with either 97810 or 97813).
Common Roadblocks to Successful Acupuncture Billing
The medical billing and coding process is complex as is without the additional requirements for acupuncture billing. For a smooth reimbursement process, it’s key to avoid these common billing challenges acupuncture practices routinely face.
Overusing Acupuncture Billing Codes
Billing an office visit every time you see a patient, or overusing codes 99205/99215, can get you red-flagged.
Incorrect Billing Use for Time
A common misconception within acupuncture billings is, because each billing code is for 15 minutes between the practitioner and patient, that an acupuncture practice can bill for four separate units of acupuncture treatment for an hour session. This is incorrect, however. Even though the initial code for acupuncture treatment (97810) is for a 15-minute interval, it also represents a dedicated set of needle-insertions, as do all the other subsequent codes. So, if your holistic practice was going to bill four units of acupuncture, there would need to be four separate needle insertions!
Using the Wrong Coding for Needles
Some acupuncture practices may be confused with the proper coding for treatments with needles. While there is a billing code for just the use of needles (A4215 needle, sterile, any size, each), needles used in a treatment session have an altogether different code.
The needle code A4215 is only accurate when a patient must take home needles for at-home home injections, the same way a diabetic patient would for insulin. Since needles are an essential part of acupuncture treatments, they cannot be billed as a separate line item. Use the acupuncture codes appropriately depending on the set of needles: 97810 initial set, manual, 97811 additional set(s) manual or 97813 initial set, electrical, and 97814 additional set(s) electrical. Using the incorrect acupuncture billing codes can delay the reimbursement process and result in denials.
Inaccurate Billing for Phone Calls
Holistic practices can bill for the time spent on the phone with patients, but there are precise individual payer reimbursement guidelines to follow that can result in payment delays if followed incorrectly. While “non-face-to-face” evaluation and management codes 99441, 99442, and 99443 can be used for phone calls, they cannot be recorded if the phone call ends with the medical decision for the patient to come to your practice within 24 hours or at the next available urgent visit time. In that case, the phone call would qualify as part of the pre-service work for the subsequent E/M service, procedure, and patient visit.
The Acupuncture Billing Terms You Need to Know
For a streamlined billing process, here are some acupuncture billing terms your holistic practice needs to be aware of.
Accounts Receivable (A/R)
One of the more common insurance billing terms you’ll encounter, A/R refers to insurance claims that have not been paid within the normal processing period. The average insurance claim pays in 30-45 days. Any unpaid claims beyond that range should be reviewed, revised, and resubmitted.
Allowed Amount
The amount of money an insurance company will reimburse you for services rendered. When billing in-network, the allowed amount will be the rate negotiated as part of your contract. If you are billing out-of-network, the rate is usually unpublished.
Annual Year Max
Commonly used with insurance benefits verifications, annual year max represents the maximum an insurance company will pay for your services during a calendar year. The amount may either be a financial sum, such as “$1,000 for acupuncture services,” or it could be a maximum number of treatments in the time period, such as “24 visits per year.”
Based on Medical Necessity (BMN)
Patients often require specific procedures to treat serious medical conditions or illnesses. These procedures are classified as “medically necessary.” Sometimes insurance companies will deny an insurance claim and request a letter of medical necessity from you. This criterion for BMN varies across insurance companies when it comes to acupuncture services. For example, one insurance company may think acupuncture treatment is medically necessary for limb pain, while others may feel it is only medically necessary for back pain.
Co-Insurance
You will see this term on most insurance verifications, usually expressed as a percentage. It refers to the portion of your service fee that the patient is responsible for paying after an insurance company pays. For example, when the insurance pays 55% of the allowable, the patient will be charged the other 45%. Thus, if the allowed amount from the payer is $100 for 30 minutes of acupuncture, the insurance will pay you $55 on the insurance claim and you will charge the patient $45.
Co-Pay
A co-pay is the amount the patient pays you at the time of service for each acupuncture treatment. The amount should be identified by your biller when verifying insurance benefits. The amount will vary depending on a patient‘s insurance plan. Usually, this will be identified in an insurance verification as an exact amount, such as $10, $25, or $50.
Medical Credentialing
This term refers to the application and negotiation process a medical or holistic practice must go through to be included in an insurance company panel or going in-network. Once you are credentialed with an insurance company, you are typically listed on the company‘s collateral materials as a participating provider for acupuncture services. This is a common process for most commercial insurance companies, medical groups, surgery centers, or government plans like Veterans Affairs, Medicare, and Medicaid.
Current Procedural Terminology (CPT)
Also known as medical coding, these numbers represent treatments and procedures performed by you as the provider during a given visit. During the acupuncture billing process, you will need to express the services rendered in CPT codes for your superbills. Any codes billed should then be reflected in the narrative of your documentation of the visit.
Date of Service (DOS)
This is the date you performed a given procedure.
Deductible
The amount of money patients have to pay out-of-pocket before their insurance benefits will subsidize payment. This amount should be identified when verifying insurance benefits. Patient deductibles are determined by their insurance plan and can range in amount.
When your client has an unmet deductible, you will typically charge the patient a fee at the time of service and then bill the claim to “run down” the deductible. Pay special attention to deductibles the first couple of months of the year because many deductibles are recalculated at the beginning of each calendar year. However, not all plans go by calendar year; some “contract year” plans use deductibles that are recalculated on a date other than January 1.
Demographics
Identifying information about a patient that is required before filing a claim. Demographic information may include things like date of birth, sex, address, and family information. An insurance company will deny a claim if it contains inaccurate demographics.
Explanation of Benefits (EOB)
This document is attached to the payment or processed medical claim wherein the insurance company explains the services it will cover for a patient‘s health-care treatments. EOBs also explain what is wrong with a claim if it‘s denied. Therefore, you always want to remit your EOBs to your biller as soon as you receive them so any issues can be resolved as quickly as possible.
Fee Schedule
A document that outlines the fees used by the insurance carrier to reimburse you for acupuncture services designated by a CPT code.
ICD-10 Codes
The 10th revision of the International Classification of Diseases coding that is used in Western medicine to diagnose medical conditions. This standard went into effect on October 1, 2015, replacing the previous ICD-9 codes. ICD-10 codes are mandatory for insurance claims for most insurance companies.
In-Network
This term refers to a contractual relationship you establish with an insurance company. To be in-network, you will need to go through the credentialing process. Plan on 90-120 days for your application to be processed by the insurance company. In-network reimbursements tend to be about a third of out-of-network reimbursements, but more patients should have in-network acupuncture benefits.
Insurance Verification Form
This is one of two primary forms used in acupuncture billing (along with the superbill). It is used to document information about a patient’s insurance information to verify coverage and benefits.
The verification form must include the patient’s name, their date of birth, the policyholder’s name, their insurance ID number, and their insurance telephone number. After this information is gathered, your acupuncture insurance biller contacts the insurance company directly and confirms the patients‘ benefits.
Maximum Out of Pocket
A cap on the amount of money a patient will have to personally pay per year (calendar or contractual) for medical services. Once the max is met, insurance pays 100% for the remainder of the year.
National Provider Identifier (NPI) Number
A unique ten-digit number ascribed to every healthcare provider in the United States, as mandated by HIPAA. Each provider in your practice will need a Type 1 Individual NPI number to bill insurance claims. If your practice has a Tax ID (TIN) or Employer ID (EIN) number, you will also need a Type II Organizational NPI number.
You can apply for either number online with the National Plan and Provider Enumeration System (NPPES).
Out-of-Network
“Out-of-network billing” refers to a relationship with an insurance company where you are considered to be outside the established network of providers that contract with an insurance company. Typical out-of-network reimbursements are three times higher than those for in-network rates.
Superbill
This is the second of the two primary forms used in acupuncture billing. It documents information about a patient and the services rendered in a given visit. The superbill can contain demographic information and insurance information, and it must include a diagnosis (ICD-10 code) and procedures (CPT codes). Your medical biller translates information found in the superbill into an insurance claim.
Taxonomy Code
A ten-character code that identifies your provider type and area of specialization when issuing a claim to the insurance company:
- Acupuncture: 171100000X
- Chiropractic: 111N00000X
- Massage Therapist: 225700000X
Tax Identification Number (TIN)
A number assigned by the IRS for use when billing insurance and receiving payment. This number assists in keeping your business and personal income separate when filing income taxes. When you receive this number, it replaces your SSN when billing.
Write-Off
The difference between your fee for services and the amount that an insurance company is willing to pay for those services for which, nevertheless, a patient is not responsible. The write-off amount may be categorized as a “not covered” amount for billing purposes.
Streamline Your Acupuncture Billing Processes & Boost Revenue for Your Holistic Practice with HBS!

With this list of essential acupuncture billing terms to reference, your holistic practice can be better prepared for medical billing processes. Still, billing is complicated, and an acupuncture practice requires separate health insurance billing steps than a traditional medical practice. Handling all of the insurance enrollments, medical billing and coding, and SOAP documentation for an acupuncture practice can be overwhelming, but outsourcing your acupuncture insurance billing can save you time and streamline your revenue cycle management!
As an experienced acupuncture billing provider, Holistic Billing Services can help your practice navigate the intricacies of insurance billing claims to minimize denials and increase revenue. We understand the unique needs of acupuncture practices and know-how to overcome common obstacles they face when dealing with insurance providers and the complexities of medical billing and coding for holistic practices.
With a knowledgeable partner by your side, you can streamline your acupuncture billing process and get back to treating patients to help your holistic practice grow. To learn more about Holistic Billing Service’s acupuncture billing services, talk to one of our billing and coding experts today.