The Centers for Medicare and Medicaid Services (CMS) released a series of changes in 2018 to the way E/M coding would be documented and billed for reimbursement. In partnership with the healthcare billing community, we reacted swiftly to the announcement, pointing out a series of potential problems that could arise when the changes went into effect for integrative medicine practitioners. In response, CMS formed a working group to consider another way of streamlining documentation burdens without focusing away from the delivery of medically necessary care. After about a year of negotiations and planning, we are happy to report that the changes were finally released to the public as part of the 2020 Physician Final Rule.
Understanding E&M Codes
An abbreviation for “evaluation and management,” E/M codes (alternatively known as E&M codes or sometimes referred to as “office visits”) are used by private practices to bill for a range of encounters that occur between patients and physicians, therapists, or practitioners. As a subset of CPT coding (specifically, CPT code range 99201-99499), E/M codes provide three pieces of information to insurance providers for reimbursement.
- Patient Type: Indicates whether the patient is new or established.
- The setting of Service: Indicates where the healthcare services were provided. For most holistic practices, this will be an office or outpatient setting.
- Level of Service Provided: E/M coding indicates the complexity of the health services delivered. A higher value code suggests a more complex service.
Under the original E/M coding structure, the level of service was determined by a complex calculation involving three elements: patient history, physical examination, and medical decision making. Each factor required the appropriate documentation to help indicate what appropriate level of service and then to bill accordingly. While holistic practitioners could use time as a determining factor when substantial counseling or care coordination was involved, that process required them to follow a very ambiguous set of guidelines.
How Are E/M Codes Changing in 2021?
Federal E/M coding guidelines will undergo a substantial change as of January 1, 2021. These changes will specifically affect coding for office and outpatient visits (CPT codes 99201-99215), making them extremely important for holistic practices to review.
New E/M Coding Rules for 2021
- New patient level 1 code (99201) is eliminated altogether, reducing the number of levels for new patient E/M visits to four. Established patients will retain the standard five coding levels.
- History and physical examination will no longer be determining factors when identifying the appropriate level of care; this doesn’t mean documentation requirements are going away altogether. Clinically relevant history and examinations must still be documented when necessary.
- Medical decision making or time can be used to determine the appropriate level of service.
- Adjustments are made to Medicare reimbursements for E/M codes. Since only a few holistic services are eligible for Medicare reimbursements, they may not impact every practice.
What Do E/M Changes Mean for Your Holistic Practice?
The overall goal of these changes was to emphasize medical decision-making and reduce the overall volume of paperwork associated with documentation. Still, the changes could have broader consequences for many practices. Most EHR systems overly rely on multiple bullet point entries to document patient history and log physical exam results. These tend to slow down patient visits and used because it was integral to the calculation used to determine the proper level of service code for E/M billing. Since the changes coming in 2021 will focus exclusively on time and medical decision-making factors to make this decision, the electronic medical records used by holistic practices should be simplified and updated to reflect the updates and speed up documentation.
Medical decision making for E/M coding is broken down into four different types, each reflected by a specific range of CPT codes:
- Straightforward (codes 99202 & 99212)
- Low (codes 99203 & 99213)
- Moderate (codes 99204 & 99214)
- High (codes 99205 & 99215) (not recommended for holistic and integrative medicine practices.)
When making a “medical decision,” physicians or therapists must consider three distinct elements pertaining to the patient:
- Number and complexity of problems being addressed.
- Amount and/or complexity of data to be reviewed and analyzed.
- Risk of complications and morbidity or mortality of patient management.
These three elements are rated according to four escalating levels that match the four types of medical decision making. The final E/M code is determined by examining each element’s level to assess the overall complexity of the decision. In order to qualify for a “Moderate” E/M code, for instance, at least two of the three elements must be at least “Moderate.” If one element is “Low,” one is “Moderate,” and another is “High,” the final E/M code would fall somewhere in the “Moderate” range (CPT codes 99204 & 99214).
This form of decision making obviously brings some degree of ambiguity, but CMS has done its best to give clear guidelines within each element to minimize confusion. A more practical approach is for practitioners to make E/M code selections based on the amount of time they spend with patients. These guidelines are much simpler than previous versions. For example, to bill for a “Moderate” encounter with an established patient (CPT code 99214), the interaction must last between 30 and 39 minutes.
Holistic practices will have to reassess their documentation and EHR systems to ensure they’re providing the information insurance companies are looking for when evaluating E/M billing codes. By far the biggest shift will be the transition from an emphasis on patient history and physical exams, which will hopefully reduce the overall level of documentation in these categories.
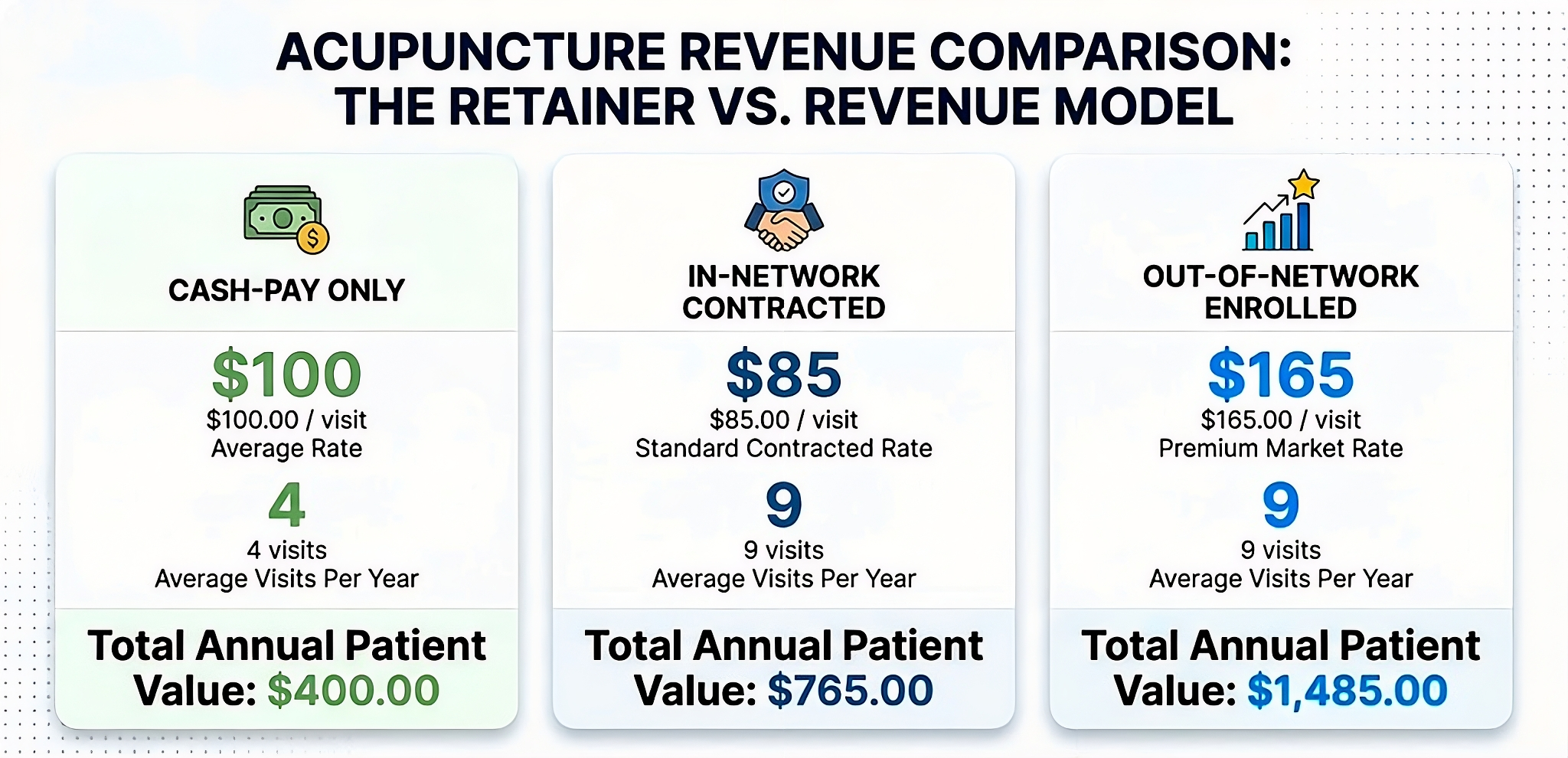
There is a lingering question about how reimbursement rates will be affected by the 2021 E/M code changes. While most holistic practices will be billing private insurers instead of Medicare, their reimbursement structure is often impacted by changes made to Medicare rates. The team at Holistic Billing will continue to monitor the situation as more information becomes available following the 2021 rollout.
Prepare Your Practice for Success with Holistic Billing!
As a medical billing specialist with a particular focus on acupuncture billing, massage therapy billing, and chiropractic billing, Holistic Billing Services has been helping independent practices adapt to new regulatory guidelines for many years. We’re always watching for the latest insurance billing announcements that could impact your holistic practice. We make sure we’re delivering the very best advice when it comes to your credentialing, billing and coding needs. If your acupuncture, massage therapy, or chiropractic practice needs help adapting to the latest round of E/M coding changes, the experts at Holistic Billing can provide the resources and guidance you need to boost your insurance reimbursements and keep your revenue cycle management moving along.
To find out what outsourced billing and coding services with Holistic Billing can do for your practice, contact our experienced team today!