Medical credentialing ensures patients receive the best quality care from credentialed providers; in other words, it’s basically an industry standard that helps maintain quality assurance. Credentialing also means that providers can file claims with various agencies, such as private insurance companies and Medicare. However, the medical credentialing process can take months and is tedious—that’s why it’s so beneficial to outsource this process. Keep reading to learn more!
What Is the Medical Credentialing Process?
Medical credentialing is vital for all new hires, but it’s also performed at regular intervals even after hiring to conform to the standards of regulatory organizations including The Joint Commission (TJC), The Centers for Medicare and Medicaid Services (CMS), and the National Committee for Quality Assurance (NCQA).
The medical credentialing process typically involves three phases and can take up 180 days:
Credentialing
During this phase, a provider’s qualifications and experience are verified and evaluated. For example, the credentialing authority—known as a Credentials Verification Organization, or CVO—will contact the university or school where the provider received their degree; this authority will also contact certification boards and licensing agencies to confirm the provider’s standing and relevant credentials. Other employers will attest to work experience as needed; essentially, this phase involves verifying the background and experience of the provider going through the credentialing process.
Privileging
This intermediate phase of the credentialing process gives the provider permission to perform specific services at the proposed institution based on your credentials being verified. Basically, the provider has been recognized for demonstrating competency in their field. Privileging is an important step because it validates your credentials and enables you to perform the services you have experience in.
Enrollment
The final component of the medical credentialing process is enrollment. This allows you, the provider, to bill and be reimbursed for the services for which you have been credentialed and are privileged to perform. Naturally, this is the end goal for holistic providers who are billing insurance companies or programs like Medicare because this phase solidifies your standing in the healthcare and holistic marketplace.
Who Can Become Credentialed?
The medical credentialing process is for any healthcare provider who needs to be credentialed in order to maintain competitiveness and be vetted for insurance or Medicare billing. A multitude of different kinds of facilities and services are obliged to acquire and maintain the proper credentials to act as healthcare providers, including:
- Durable Medical Equipment
- Home Health Services
- Hospice Care
- In-Home Care Services
- Prosthetics/Orthotics
- Radiology/Diagnostic Imaging
Essentially, the medical credentialing process can apply to any individual or entity that provides healthcare services.
Top 3 Benefits of Outsourcing the Medical Credentialing Process
While the medical credentialing process is vital for a streamlined billing experience and for a high quality experience for the patient, it’s also a tedious and time-consuming process. It involves a mountain of paperwork and can take months to complete; luckily for you, you have the option to outsource this challenging process!
The top three advantages of outsourcing the medical credentialing process for your holistic provider include:
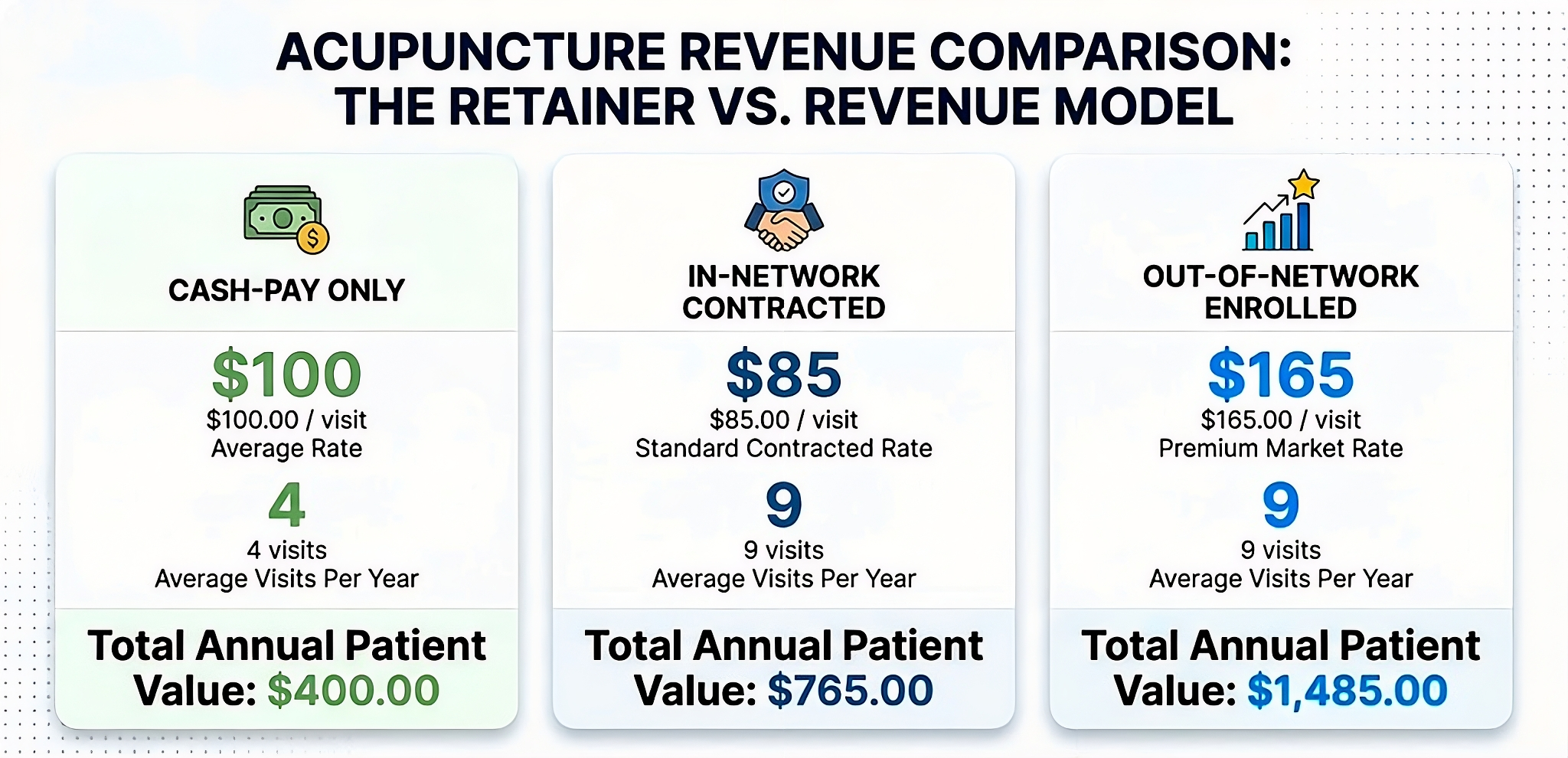
Your H Practice Can Accept Patients with Insurance and Medicare
Being able to accept patients who carry insurance or are supported by Medicare is a game changer for your holistic practice! Medical credentialing helps make this happen; private insurance companies, as well as government programs like Medicare, have an incentive to minimize the costs of their operations and part of this results in only working with providers who are credentialed. Credentialed professionals and providers demonstrate verified competency in their field and, therefore, pose minimal risk. Overall, the medical credentialing process further recognizes and validates your authority to deliver high quality care to members of your community.
It Enables Your Team to Handle Other Important Matters
Chances are you, as well as each member of the team at your holistic practice, wear many hats; this means you’re balancing administrative work with customer service all while delivering great care to your clients. The medical credentialing process is a significant undertaking that would further deplete your team’s time and efforts that might be otherwise better spent elsewhere. By outsourcing the medical credentialing process, you and your team can continue to support every other initiative at your holistic practice while a team of experts handles your important credentialing journey.
It Ensures Accuracy Following the Credentialing Process
What good is completing the medical credentialing process if the application has missing, outdated, or inaccurate information and has to be done again? Not much! Overlooking significant aspects of the medical credentialing application can result in significant delays and overall frustration for your holistic practice. Postponed credentialing means postponed opportunities to serve patients with insurance or Medicare, which essentially impacts your revenue cycle.
Furthermore, each state is likely to have different credentialing regulations and requirements. Not understanding your state’s regulations can also throw a wrench in the medical credentialing process. Outsourcing this process, however, means you don’t have to worry about inaccuracies or misunderstandings!
Outsource Your Medical Credentialing Process with Holistic Billing Services!
Medical credentialing maintains and perpetuates confidence in the quality of healthcare providers and works to keep costs down; medical credentialing is a win-win for everyone involved! If you need to gain or update your medical credentials but don’t want to deal with the headache of completing the process yourself, then let Holistic Billing Services handle it for you!
Our team of experts will ensure accuracy and navigate the process for you so that you and your holistic practice can continue doing what you love: serving your community! Contact us today to learn more!